| Table of Contents |  |
|
Original Article
| ||||||
| Detection rate of incidental findings and vestibular schwannomas on magnetic resonance imaging scans investigating unilateral audiovestibular symptoms | ||||||
| James Andrew Douglas1, Matthew James Lee2, Osama Al Hamarneh3, Christopher Coulson4 | ||||||
|
1MRCS DO-HNS, Core Surgical Trainee, Department of Otolaryngology, Queen Elizabeth Hospital, Birmingham, UK.
2MRCS, Core Surgical Trainee, Department of Otolaryngology, Queen Elizabeth Hospital, Birmingham, UK. 3FRCS ORL-HNS, Senior Registrar, Department of Otolaryngology, Queen Elizabeth Hospital, Birmingham, UK. 4PhD FRCS ORL-HNS, Consultant in Otolaryngology and lateral skull base Surgeon, Department of Otolaryngology, Queen Elizabeth Hospital, Birmingham, UK. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Douglas JA, Lee MJ, Al Hamarneh O, Coulson C. Detection rate of incidental findings and vestibular schwannomas on magnetic resonance imaging scans investigating unilateral audiovestibular symptoms. Edorium J Otolaryngol 2014;1(1):1–6. |
|
Abstract
|
|
Aims:
Establishing the rate of detection of vestibular schwannomas and incidental findings on magnetic resonance imaging scans of the internal auditory meatus for investigating asymmetrical sensorineural symptoms, and see if there is a difference between types of center investigating these symptoms.
Methods: Retrospective review in two trusts, one district general hospital and one tertiary hospital over a two-year period. All primary scans were reviewed. Results: The number of identified scans was 2174. Vestibular schwannomas were diagnosed in 1.7% (n=11) at district general hospital and 1.4% (n=21) at tertiary hospital. Incidental findings more common in tertiary hospital (39.9% vs 24.5% in district general hospital, p=<0.0001), most frequently ischemia (15.8%) and sinus disease (5.2%). Serious incidental findings were detected in 2.4% of scans. No abnormality detected in 1407 scans. Conclusion: The pickup rate was not significantly different between district general hospital and tertiary hospital. High rate of incidental findings was seen, however, most did not require follow-up. Higher rate of abnormalities was detected in tertiary hospital associated with availability of neuroradiologists. The availability of neuroradiologist was useful when counseling patients prior to investigation. | |
|
Keywords:
Acoustic, Vestibular schwannoma, Audiovestibular symptoms
| |
|
Introduction
| ||||||
|
Cerebellopontine angle (CPA) tumors are the most common neoplasms in the posterior fossa, accounting for 5–10% of all primary intracranial tumors. Most posterior fossa tumors are benign meningiomas, which account for 13–25% of all primary intracranial tumors. [1] However, when looking specifically at the CPA, roughly 80% are vestibular schwannoma. [2] Meningiomas and epidermoids account for 10% and 6%, respectively with lipomas, vascular malformations, hemangiomas and lower cranial nerve schwannomas accounting for the remainder. [2] [3] A vestibular schwannoma classically presents with unilateral or asymmetrical sensorineural hearing loss (SNHL), often in the high frequencies and accompanied by poor speech discrimination. [4] Speech audiometry however, is not routinely performed in audiology departments in the UK. Diagnostic imaging is, therefore, offered to these patients to rule out vestibular schwannomas as a cause of their asymmetrical hearing loss. Asymmetrical tinnitus, asymmetrical bilateral hearing loss, true vertigo, disequilibrium and trigeminal nerve distribution paresthesia are also indications for diagnostic imaging. [5] Magnetic resonance imaging of the internal acoustic meatus (MRI IAM) scan with gadolinium enhancement is the gold standard to investigate lesions in the internal acoustic meatus and CPA. [6] Whilst it is possible to identify these lesions on computed tomography (CT) scans, in over 50% of patients [7] this modality often only raises suspicion by demonstrating an area of smooth bony erosion. Furthermore, establishing exact anatomical location and distinguishing between normal brain parenchyma and tumor tissue is more accurate on MRI scan than CT scan. [8] During the imaging process the cerebral hemispheres, cerebellum, brain stem and more superficial structures are all analyzed. It is, therefore, inevitable that either no abnormality will be detected on imaging or lesions not attributable to the symptoms being investigated may be identified. One systematic review by Morris et al. looking at incidental findings on MRI scan of healthy individuals showed a 0.7% prevalence of a neoplastic incidental brain finding and 2.0% a non-neoplastic one (excluding microvascular disease). Specifically, 0.03% of patients without symptoms were found to have vestibular schwannomas. [9] Wong et al. looked into findings on MRI scans performed in one district general hospital and described that incidental findings were present on 46.7% of patients. [10] In our region, patients with a CPA tumor are referred to a tertiary centre for joint neurosurgical and otolaryngology care. Given this, it seems pragmatic to determine if the detection rate of tumors and incidental findings are different depending on where investigations are performed. Ultimately, after a normal or abnormal scan, the question then arises of how to proceed; one study suggests with appropriate prior counseling, over 50% of patients requiring MRI IAM do not require ENT follow-up. [11] The aim of this paper is to determine the detection rate of incidental findings on MRI IAM at both a district general hospital (DGH) and a tertiary hospital (TH) and to establish the pickup rate of vestibular schwannomas in these two types of hospital. | ||||||
|
Materials and Methods
| ||||||
|
Data were collected retrospectively from two trusts; one tertiary centre and one district general hospital. A list of all MRI IAM scans performed for audiovestibular symptoms was acquired from the hospitals' imaging viewing and reporting systems for a two-year period (January 1, 2008-December 31, 2009). All reports were reviewed and indications for scanning and findings recorded. Any missing indications were extracted from clinic letters. Only the first scans for new symptoms were included; all monitoring scans of previously diagnosed tumors were excluded. Statistical analysis was performed using Graph Pad Prism 6 (Graph Pad Software, San Diego). The study gained approval from the local audit and governance departments in each hospital. Definitions | ||||||
|
Results | ||||||
|
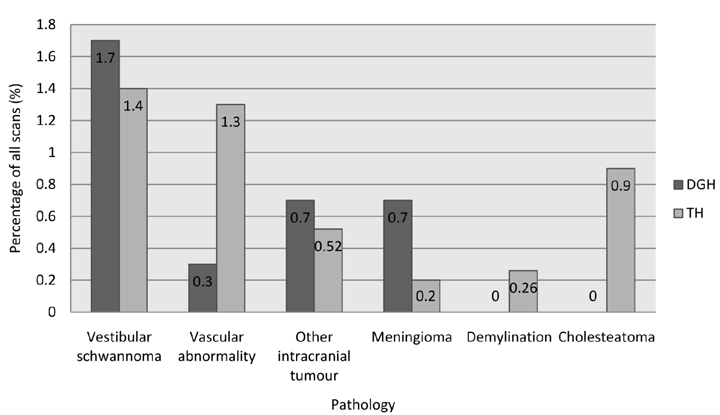
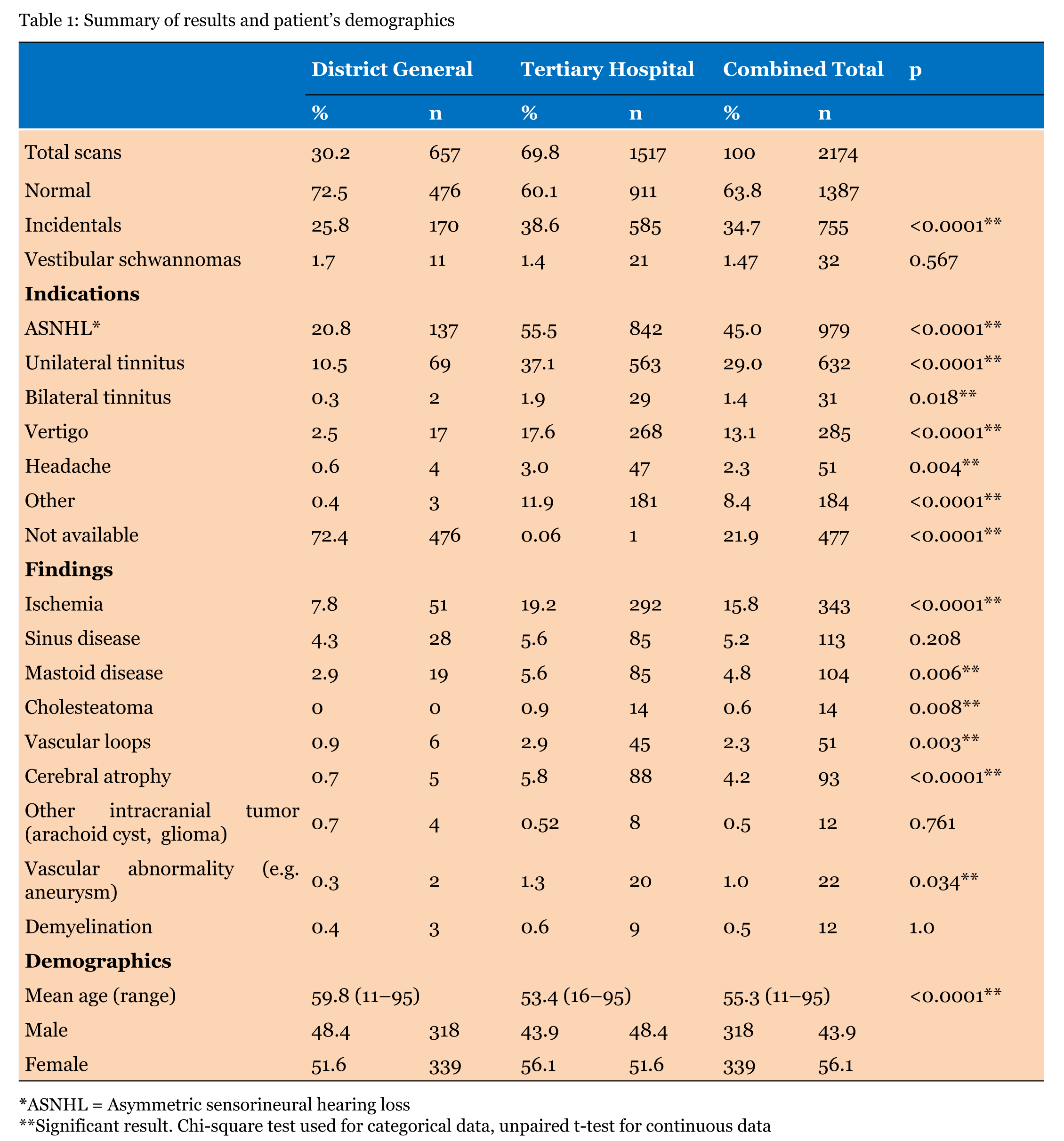
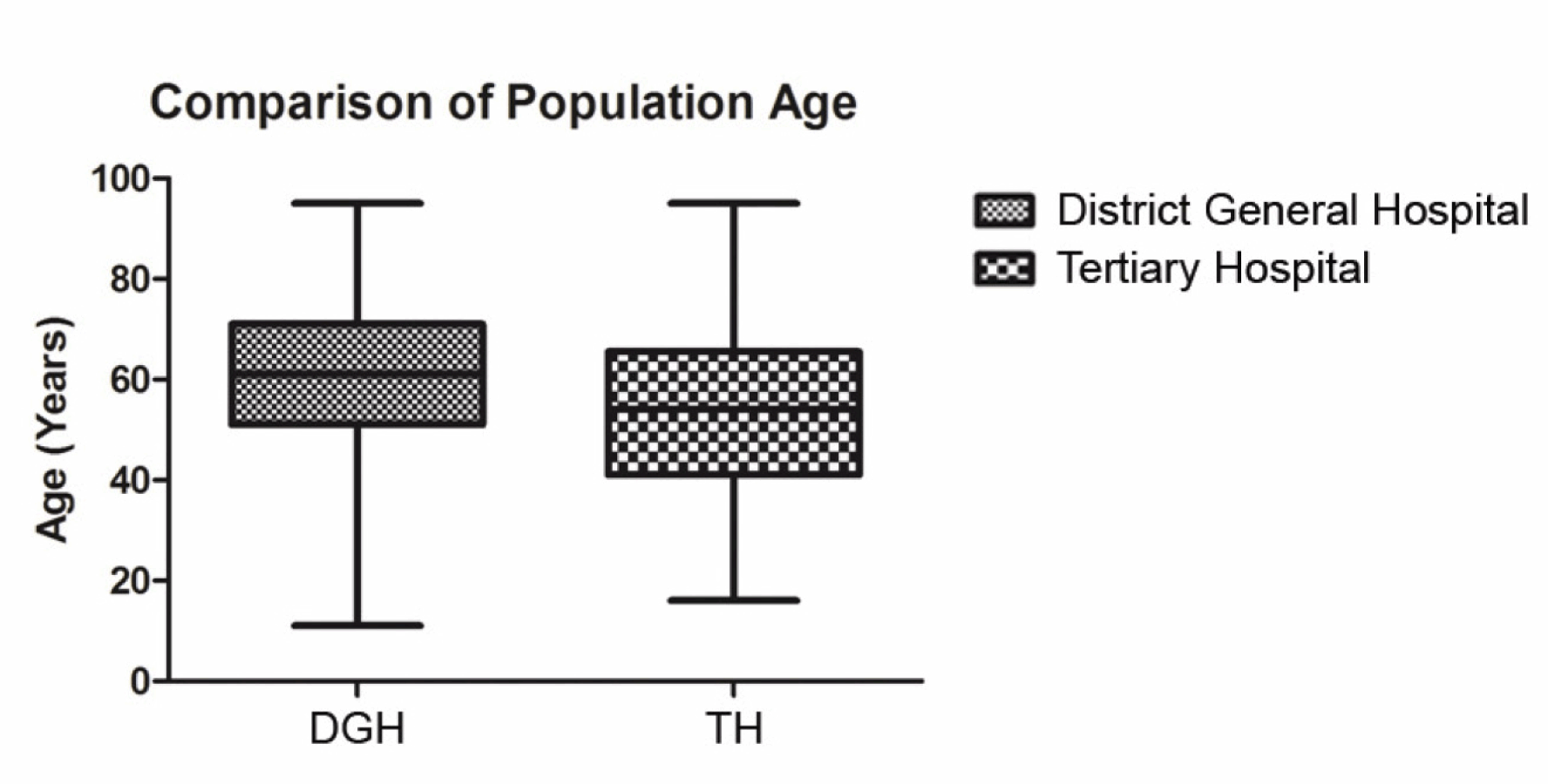
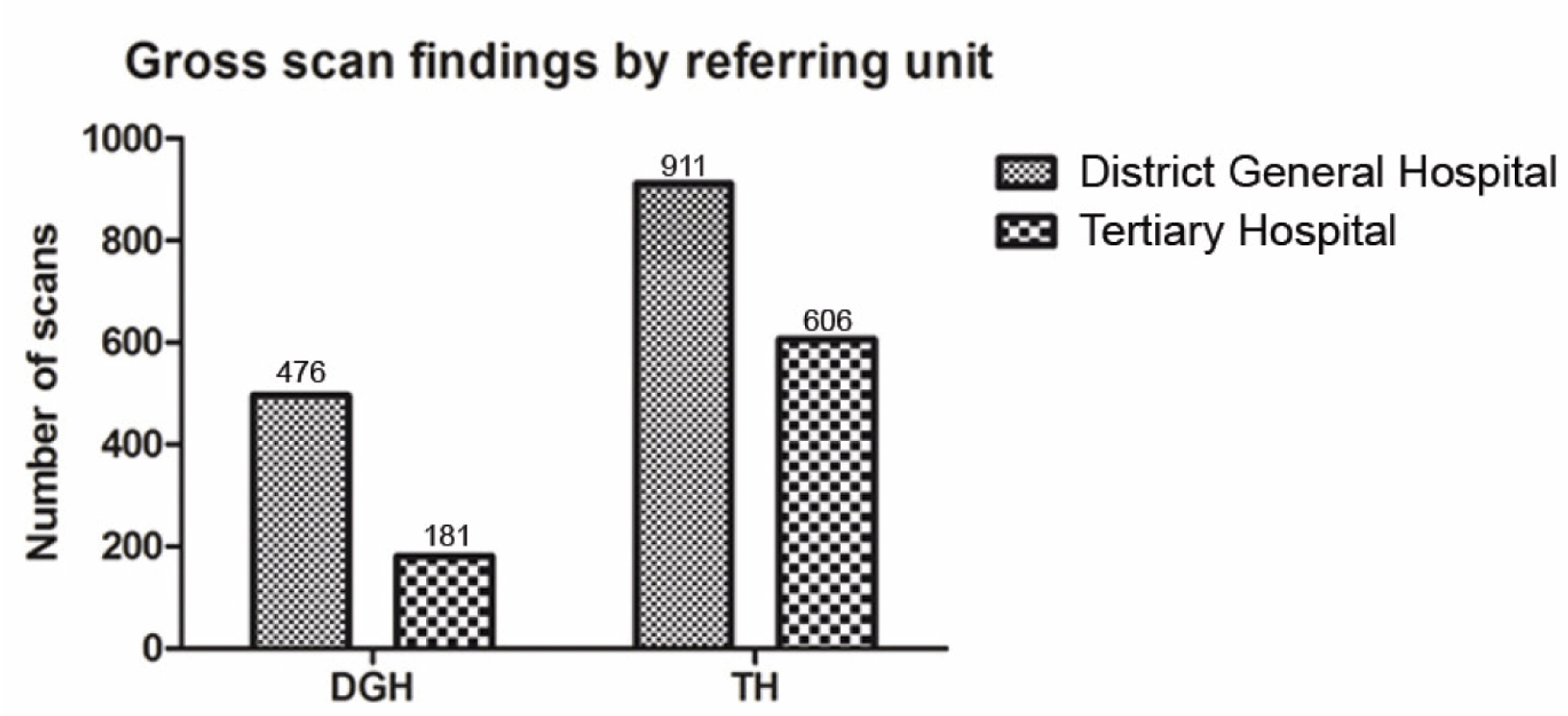
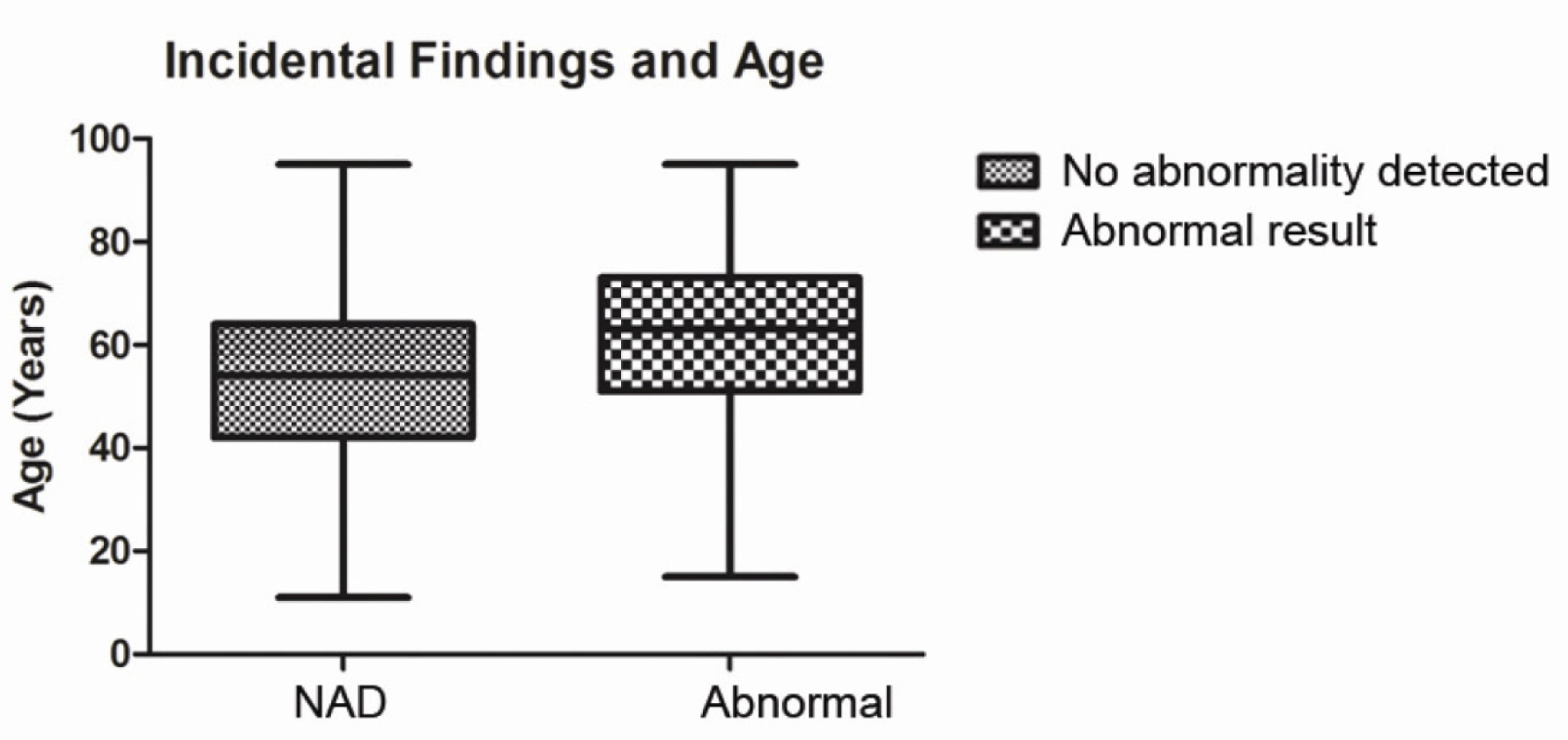
District General Hospital: The number of scans taken place in the DGH during the study period was 657 in which 339 patients were female and 318 were male. The mean age of patients scanned was 59.8 years (range 11–95 years). No abnormality was detected following 476 (72.5%) scans. Incidental findings were found in 170 scans (25.8%). The most frequent incidental findings were evidence of ischemia in 51 scans, sinus disease in 28 scans and mastoid disease in 19 scans. Vascular loops, meningioma and arachnoid cyst were also seen. (Figure 1) Vestibular schwannoma was diagnosed on 11 scans (1.7%). (Table 1) All scans were authorized by a consultant radiologist. Tertiary Hospital: The number of scans taken place in the TH during the study period was 1517 in which 851 patients were female and 666 were male. The mean age of patients was 53.4 years (range 16.1–95.1 years). No abnormality was detected following 911 (60%) scans. Incidental findings were found in 585 scans (38.6%). The most frequent incidental findings were ischemia in 292 scans, sinus disease in 85 scans and mastoid disease in 85 scans. Vascular loops, meningioma, arachnoid cyst and other space occupying lesions were also seen. (Figure 1) Vestibular schwannoma was diagnosed on 21 scans (1.4%). All scans were authorized by a consultant neuroradiologist. Comparison Incidental findings were associated with a higher average age (52.5 vs 60.3 years, Mann-Whitney U test p < 0.0001, (Figure 4) but not with gender (chi-square test p = 0.924). Comparison of the rates of diagnosis of vestibular schwannomas between DGH and TH showed no significant difference (11 vs 21, chi-square test p = 0.6). Caution should be exercised in comparison of indication for scans between units due to the large amount of missing data from the DGH. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
In this study, the detection rate for incidental findings on MRI IAM scan for unilateral audiovestibular symptoms was found in over a third of all scans at two different hospitals (34.7%). Vestibular schwannoma detection rate was 1.47%. The results of this study demonstrates that a tertiary hospital (TH), when compared to a district general hospital (DGH), accounts for a greater pick up rate of incidental findings but similar rates in detecting vestibular schwannomas . The majority of incidental findings in both groups is small vessel/ischemic type change. It does not seem to be a clinically important difference. If this group of findings is ignored, the pickup rates of other potentially more significant findings are comparable between the two units. As there is not a universal protocol to report the scans, it is at the radiologist's discretion to mention less clinically significant incidental findings. All scans were reviewed by a consultant radiologist at the DGH and neuroradiologist at the TH. Both hospitals used 1.5 Tesla scanners and comparable protocols (1 mm slices through the IAM and 5 mm for rest of brain at the DGH and 1.5 mm slices through the IAM and 5 mm for rest of brain at the TH). The increased reporting of incidental findings may reflect the specialist presence at the TH. A recent review of 200 MRI IAM scans in a population undergoing investigation for audiovestibular symptoms had an incidental finding rate of 47.5%, [12] while another study by Wong et al. found 46.7% (n = 396) [10] which are both higher than our report (34.7%). The population in our study included a younger age range than in other studies, (11–95 vs 53–92 [10] and 17–82) [12] years and thus our rates of ischemia were lower (15.8% vs 26.5% [10] and 33%) [12] which may account for this difference. As reported previously, our results showed that abnormalities on MRI IAM scan are associated with increased age, the majority of which were ischemic or small vessel disease changes. [9] [13] The TH involved in this study does not provide pediatric services so we would expect this population to have a higher mean and median age, however, this is not the case. With current practice, the pickup rate of vestibular schwannomas on MRI scan is less than 2% (TH 1.4%, DGH 1.7%). This rate showed no significant difference between the two hospitals in this study. There are no universal applied guidelines on whom to scan when investigating patients with audiovestibular symptoms. However, Obholzer et al. showed using a scan criterion of 15 dB or more inter-aural difference in two adjacent frequencies are used, if the mean threshold in the better ear was <30 dB, and 20 dB if greater than 30 dB on pure tone audiogram, sensitivity is increased to 97% and number of scans requested for these symptoms is reduced by 44%. [5] The consistent vestibular schwannoma pickup rate across the two hospitals are similar to previously reported diagnostic rates [14]and these values will be useful when counseling patients about the likelihood of diagnosing vestibular schwannoma when undertaking an MRI scan. Importantly for patients, the type of unit performing MRI scans does not seem to determine the likelihood of clinically significant pathology being detected. The other factor to consider is whether it is appropriate to discuss all incidental findings with patients especially as many are asymptomatic or considered normal changes for age. In cases where carotid aneurysm or glioma was found, a neurosurgical referral was made. Advice exists for the follow-up and management of meningiomata and arachnoid cysts. [15] Knowledge of the management of incidental findings is important for two reasons; firstly, due to the pickup rates of vestibular schwannomas and incidental findings, we are more likely to make an incidental finding on imaging than to diagnose vestibular schwannomas. Secondly, incidental findings are more common in older patients and demographics are shifting, reflecting an older society. We recommend that units carrying out MRI IAM scans should have a policy outlining the follow-up and management of the most common or serious findings. | ||||||
|
Conclusion
| ||||||
|
In conclusion, this study demonstrates the detection rates of incidental findings and vestibular schwannomas in a tertiary hospital and a district general hospital in the UK. The study compares pickup rate of clinically significant and insignificant incidental findings at different types of hospital and discusses their nature and management. Whilst we have shown there is a disparity in either the true incidence or reported rate of clinically insignificant incidental findings, importantly there is no difference in detection rates of clinically significant ones. We believe that the results from this report are most useful when counseling patients before and after receiving diagnostic imaging. | ||||||
|
Acknowledgements
| ||||||
|
Dr Sarah Dawes, House Officer, Department of Otolaryngology, Queen Elizabeth Hospital, Birmingham, UK. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
James Andrew Douglas – Acquisition of data, Drafting the article, Critical revision of the article, Final approval of the version to be published Matthew James Lee – Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Osama Al Hamarneh – Conception and design, Acquisition of data, Critical revision of the article, Final approval of the version to be published Christopher Coulson – Conception and design, Critical revision of the article, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2014 James Andrew Douglas et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|